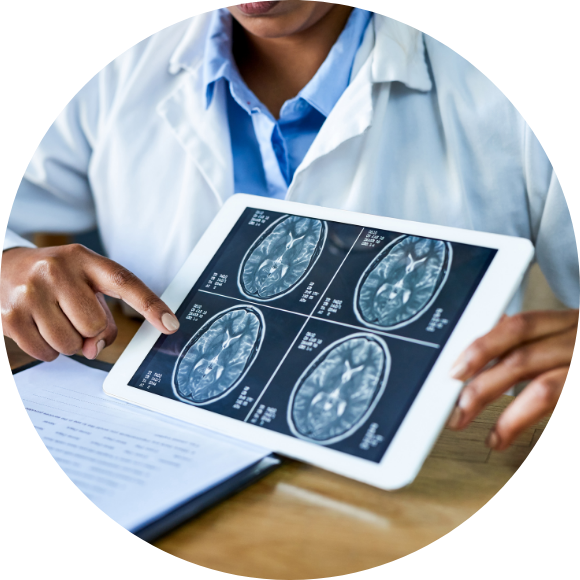
Discover education, supportive care tips, and navigation insights from our team.
Brain Tumor Education
Learn how brain tumors can affect the body and mind, from early warning signs to statistics on who is most impacted. Clear, plain-language guides help patients and families know what to watch for and what questions to ask.

Why a Second Opinion Matters
Learn why getting a second opinion in brain tumor care can change your treatment decisions and strengthen your confidence moving forward.
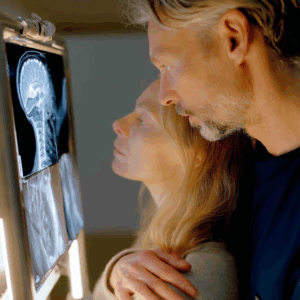
5 Steps After Brain Tumor Recurrence
Facing a recurrence? Get five key steps to guide your next move with clarity and strength.

5 First Steps After a Brain Tumor Diagnosis
After a brain tumor diagnosis, start strong with five clear actions to support treatment planning and peace of mind.

Understanding Brain Tumor Biomarkers
Get clear explanations of brain tumor biomarkers and how they can guide treatment and care decisions.

AYA Brain Tumor Statistics
Discover what the data says about brain tumors in teens and young adults and what this means for patients and caregivers.

Common Signs and Symptoms of a Brain Tumor
Know the warning signs of a brain tumor so you can act early and get the care you need with confidence.
Supportive Care, Palliative Care & Family Resources
Explore practical tools and approaches that make life with a brain tumor a little more manageable. From palliative care to kid-friendly education, these pieces focus on comfort, communication, and support for the whole family.

The Critical Role of Neuro-Oncology Navigators
See how neuro-oncology navigators help patients and caregivers make sense of a brain tumor diagnosis with steady support and clear guidance every step of the way.

Brain Tumors Decoded: A Complete Guide
Get clear, patient-friendly answers to brain tumor basics, tests, treatments, and support all in one place.

Why Palliative Care Matters
Many people hear “palliative care” and think it means giving up. It doesn’t. It’s a medical service that focuses on your comfort, your goals, and your daily life.

Introducing “Coloring Cancer: A Colorful Way to Understand Brain Tumors”
Coloring Cancer is a free coloring book designed to help families talk openly and stay connected.
BTN News and Updates, Partnerships, & Recognition
Stay up to date on Brain Tumor Network’s milestones, new partnerships, and organizational achievements. Learn how our board, collaborators, and national recognition all support stronger services for patients and caregivers.

Dr. Susan Chang Joins BTN Board
Meet Dr. Susan Chang, the newest member of Brain Tumor Network’s board and a strong voice for patient and caregiver support.

Leading the Way in Oncology Navigation
Learn how Brain Tumor Network is advancing oncology navigation with patient-first care and trusted support.

Expanding BTN’s Impact
See how Brain Tumor Network is growing its support and reach to help more patients and caregivers every day.

Patient Advocacy: A Global Perspective
Explore how patient advocacy shapes brain tumor care worldwide and why your voice matters.

BTN Celebrates 10 Years of Patient Navigation
Celebrate 10 years of Brain Tumor Network’s navigation support and see how steady help has made a real difference for patients and families.

BTN Expands Navigation Support Through Strategic Collaboration With American Cancer Society
A new collaboration with the American Cancer Society makes it easier for people with brain tumors and their caregivers to get free, expert navigation support from Brain Tumor Network.